Pediatric Physical & Occupational Therapy
in Birmingham, AL & Houston, TX
Welcome to PhysioBaby Therapy & Wellness

Our expert therapists specialize in holistic, manual therapy techniques designed to support the unique developmental needs of infants, young children, and their families. We offer hands-on care at our clinic in Birmingham, Alabama, and concierge in-home therapy for families in Houston, Texas.
Call today to book a personalized evaluation and experience the PhysioBaby difference from the very first visit.

Our Therapy & Wellness Services for Children & Families
We use our hands-on skills to set little bodies up for success and optimal function. To support this goal, we offer a variety of specialized treatments designed to meet your family’s unique needs:

Pediatric Physical Therapy
Our pediatric specialists help your child improve mobility, strength, and coordination through hands-on manual therapy. We create individualized treatment plans to prepare your child’s body to achieve its ultimate function for a lifetime of independence.

Pediatric Occupational Therapy
We support your child’s fine motor skills, sensory processing, and ability to engage confidently in daily activities. Our occupational therapists use hands-on techniques to help your child gain the functional skills they need to successfully participate in daily tasks.

Pediatric Feeding Therapy
Our team supports families with young infants who are learning to nurse or bottle-feed. We offer personalized guidance to help make feeding more comfortable, effective, and enjoyable for both you and your baby.

Tethered Oral Tissue (TOTs) Therapy
We offer expert care before and after tongue- or lip-tie release procedures to optimize your child’s outcomes post frenectomy. Our therapists provide comprehensive support through gentle, hands-on techniques to support your child’s overall wellness, comfort, and successful outcomes.
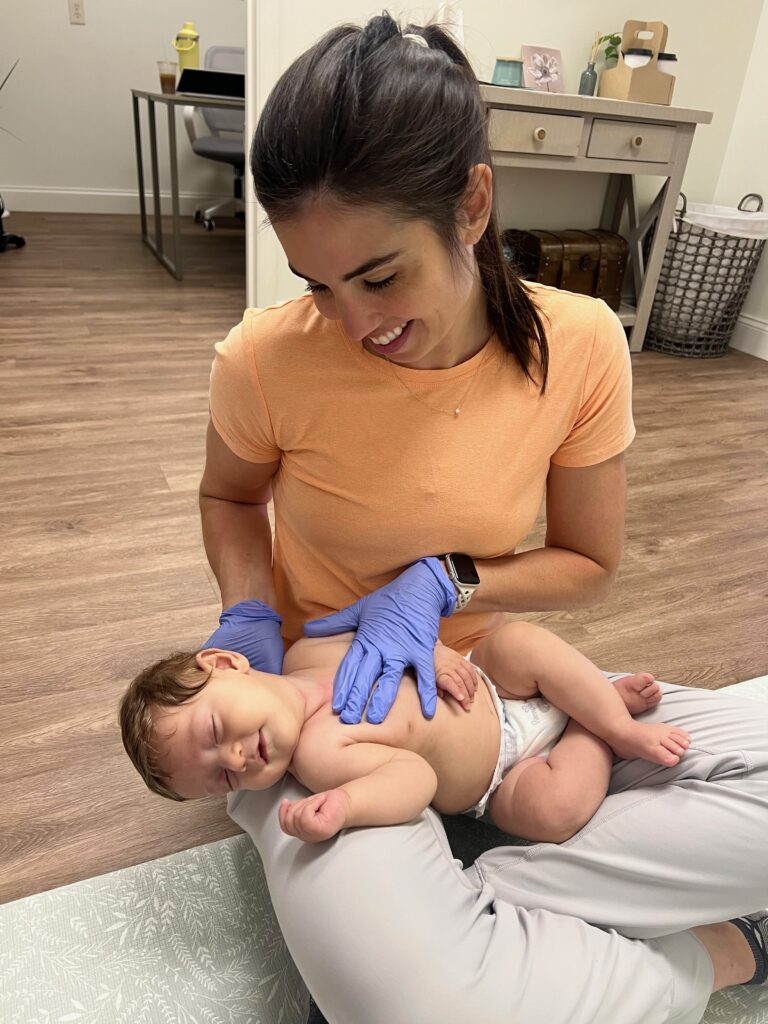
Craniosacral Fascial Therapy (CFT)
Our therapists use gentle, hands-on techniques to address birth trauma, head shape, colic, and many more conditions in infants and young children. This holistic approach restores balance and promotes overall physical and emotional health. It also offers incredible benefits for our adult patients.
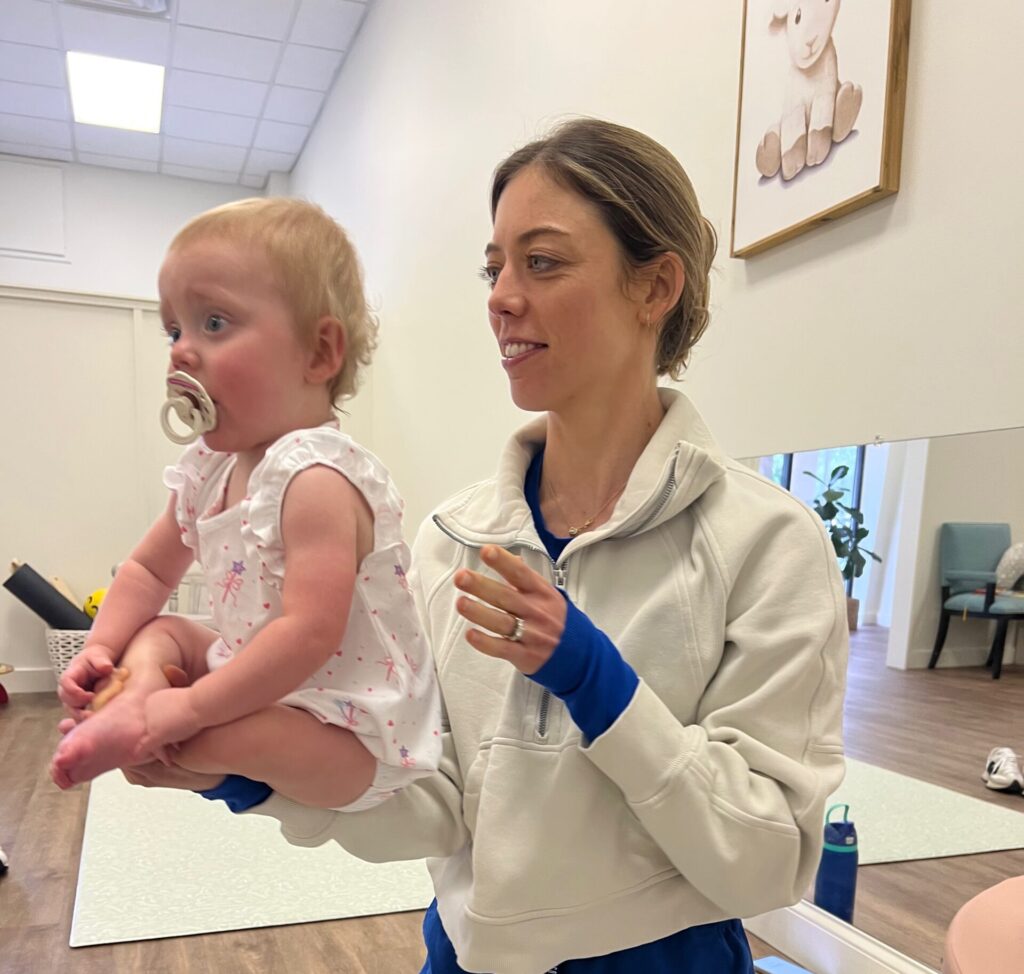
Dynamic Movement Intervention (DMI)
This innovative approach to pediatric therapy helps children build strong movement patterns and overcome gross motor skill delays. We use gentle, customized exercises designed to strengthen your child’s ability to move, explore, and play independently.
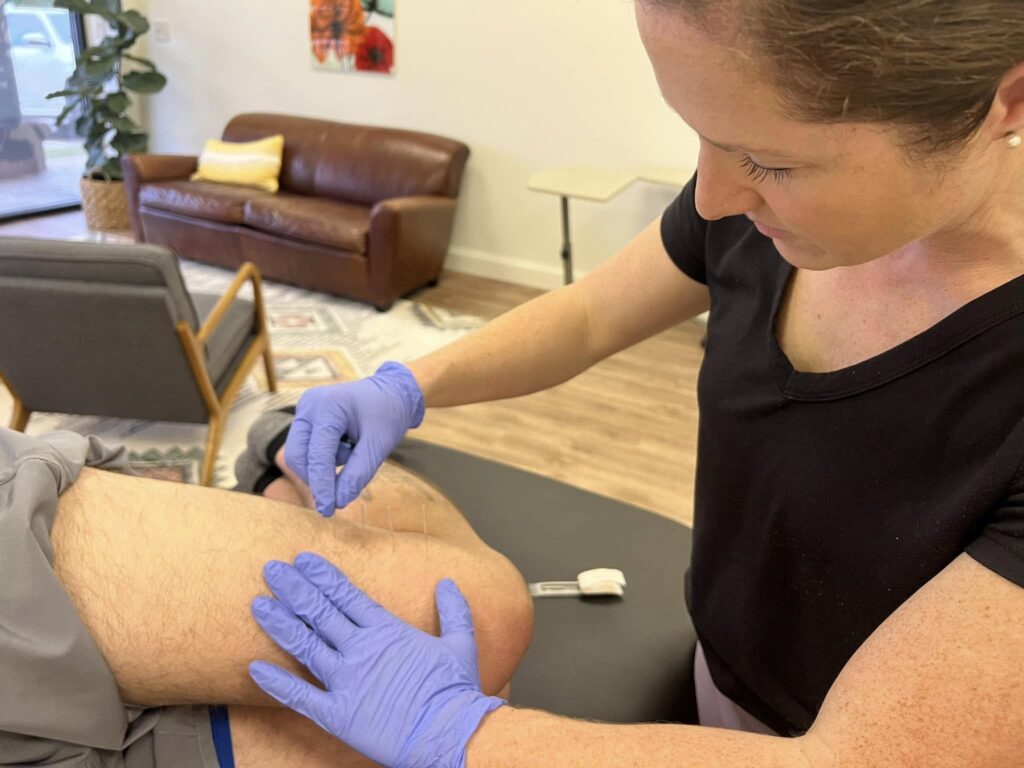
Dry Needling for Adults
Our skilled therapists can help you find relief from muscle pain and tension through dry needling. This proven technique helps decrease myofascial tightness, improve blood flow, and reduce musculoskeletal pain.

Therapy for the Whole Family
We offer specialized treatments for parents and caregivers to restore your comfort and mobility so you can better support your child’s development. Our hands-on, orthopedic approach can relieve pain, strain, and minor injuries that happen when caring for the smallest members of our families.
About PhysioBaby Therapy & Wellness
Our team is made up of pediatric experts who believe big breakthroughs begin with small steps. We start by addressing the body’s structure through hands-on manual therapy and orthopedic care, then focus on achieving optimal functional movement patterns to help each child reach their full potential.
We also offer niche and alternative treatment methods to help infants, children, and families achieve the best possible outcomes. And many of our therapists have extensive hospital experience working with medically fragile infants, which means we can provide the highest level of care to meet your child’s needs.
Families choose us because our clinic is a safe, judgment‑free place where we offer genuine support and celebrate every inch of progress right alongside you.

About PhysioBaby Therapy & Wellness
Our team is made up of pediatric experts who believe big breakthroughs begin with small steps. We start by addressing the body’s structure through hands-on manual therapy and orthopedic care, then focus on achieving optimal functional movement patterns to help each child reach their full potential.
We also offer niche and alternative treatment methods to help infants, children, and families achieve the best possible outcomes. And many of our therapists have extensive hospital experience working with medically fragile infants, which means we can provide the highest level of care to meet your child’s needs.
Families choose us because our clinic is a safe, judgment‑free place where we offer genuine support and celebrate every inch of progress right alongside you.
Is Your Child Reaching Their Developmental Milestones?

Not sure if your child needs pediatric therapy? Take our free online developmental screening! This is a private, fast way to gain certainty on your child’s development.
In just a few minutes, you’ll receive clear feedback on your child’s motor, feeding, and play milestones. Plus, we’ll give you practical next steps to know how you can help your child flourish.

Testimonials from Our Families
… We have worked with all 3 therapists and they are all amazing. This service was also covered by our insurance which we were unaware that it would be. They have helped us with feeding issues, muscle tightness, torticollis, and so many other things. We highly recommend them to anyone looking for a service. What we thought was "colic" turned out to be discomfort that was resolved once we got our baby the help she needed at PhysioBaby. We love them so much!” - Maddie
Schedule an Evaluation with Our Team Today
Our team of pediatric specialists is ready to provide expert care for your child. During the evaluation, we’ll show you what we see, why it matters, and outline a practical therapy plan you can start right away.
Give us a call to schedule an evaluation, and let’s work together to give your child and your family the support you deserve today.


